“Our Patients Come First.”
Sinus & Sinusitis in Baltimore, MD
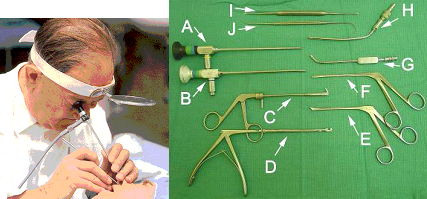
Our goal at the Maryland ENT is to offer high-quality treatment to our patients. We focus on medical and surgical rhinology and related disciplines for both adults and children. Some of our medical treatments include:
- Nose ailments
- Sinus disorders
- Olfactory disorders
- Nasal allergy
- Functional nasal surgery for nasal obstruction
- Minimally invasive endoscopic sinus surgier
- Balloon sinuplasty
- Cosmetic nasal surgery
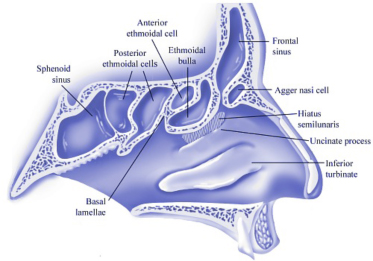
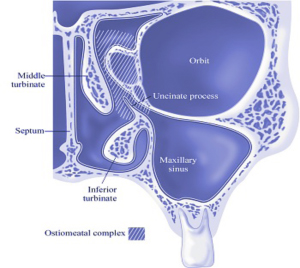
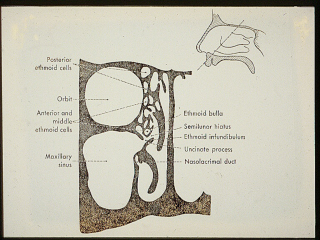
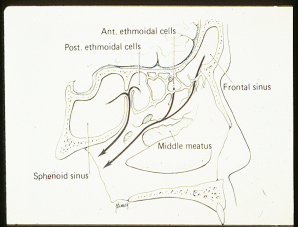
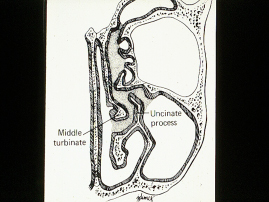
The physicians at Maryland ENT are known for their work in and Rhinology, nationally and internationally. Rhinology, Greek for “rhinos” or “nose”, is the study of the nose and sinuses. Rhinology handles all medical and surgical diseases of the nasal passages as well as paranasal sinuses.
About Our Physicians
The physicians of the Maryland ENT, inlcuding Dr Gol, have published numerous articles and publications in peer review journals and books, and made numerous presentations in national and international meetings, including the American Academy of Otolaryngology national meetings and specialty rhinology meetings in the US and around the world.
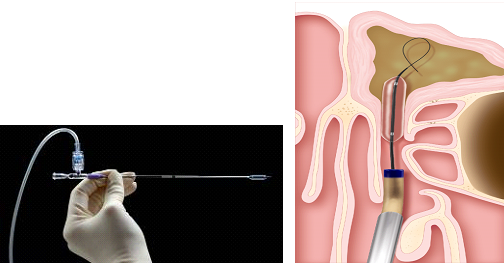
What is Balloon Sinuplasty?
Sinus Symptoms
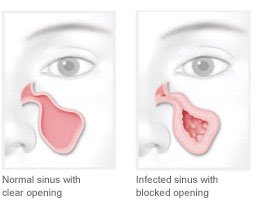
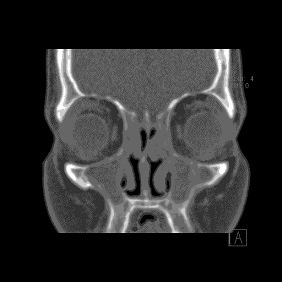
Sinusitis (also called rhinosinusitis) is an inflammation of the sinus lining that prevents normal mucus drainage through the nose. This blockage causes mucus to build up in the sinuses and can lead to very uncomfortable symptoms. Sinusitis symptoms may include:
- Sinus pressure and congestion
- Sinus Headache
- Facial pain
- Tenderness and swelling around the eyes, cheeks, nose and forehead
- Difficulty breathing through the nose
- Loss of the sense of smell or taste
- Yellow or green mucus from the nose
- Teeth pain
- Fatigue
- Sore throat from nasal discharge
- Bad breath
Balloon Sinuplasty In-Office
Office-based sinus dilation may be a compelling option for patients who decline or are ineligible for traditional OR-based surgery. With Balloon Sinuplasty In-Office, the majority of patients return to normal activity within two days of the procedure.
Balloon Sinuplasty In-Office – Clinical Benefits to an Expanded Patient Population
- Restore normal sinus drainage and function without bone or tissue removal, which preserves future treatment options
- Consider the opportunity for earlier intervention when medical therapy has failed
- Perform Balloon Sinuplasty In-Office procedures within a comfortable office setting under local anesthetic
- Lower the financial burden for eligible patients (reduced copay and procedural costs)
Do you struggle with congestion or have difficulty breathing through your nose? If other treatments haven’t helped, you may be a suitable candidate for a treatment called RhinAer, now offered at Maryland ENT.
What is RhinAer?
RhinAer is a non-surgical treatment for patients with difficulty breathing through their nose. RhinAer can treat both runny noses and congestion.
It’s designed for patients with chronic rhinitis. Chronic rhinitis is a common condition that millions have but are often undiagnosed. Chronic rhinitis symptoms include a constantly runny nose, persistent post-nasal drip, always feeling stuffed up, and excessive sneezing.
How Does RhinAer Work?
Before your RhinAer treatment, your ENT specialist at Maryland ENT will apply local anesthesia to numb the inside of your nose to ensure you don’t feel any pain and are comfortable. Then, they will insert the small RhinAer wand into your nostril.
The wand uses low-temperature radiofrequency (RF) energy from the tip. The radiofrequency energy targets and calms down overactive nerves in your nose, which helps reduce the production and flow of unwanted mucus being created.
In addition to calming down overactive nerves, RhinAer can also shrink any inflamed soft tissue in the nose. Doing this helps relieve congestion, making you feel more comfortable.
Once your RhinAer treatment is complete, you can return to your usual activities since there’s minimal downtime. However, each patient is different, so your results may vary.
RhinAer’s console can also be used with the VivAer Stylus for patients with nasal airway obstruction. Combining RhinAer and VivAer provides lasting relief to these patients by treating the entire nasal valve.
Who is a Good Candidate for RhinAer?
RhinAer is best suited for patients suffering from chronic rhinitis symptoms. You may be a good candidate for RhinAer if:
- You suffer from a moderate to severe chronically runny nose
- You have post-nasal drip
- You’re always congested
- You suffer from chronic clearing of your throat
- You have had Functional Endoscopic Sinus Surgery (FSS) but still suffer from uncontrolled rhinitis
- Medications and nasal sprays aren’t providing you with the relief you need from your frustrating symptoms
- You have allergies that cause constant drainage
RhinAer is only for use by adults who are at least 22 years of age and older.
If this sounds like you, you may be a good candidate for RhinAer. However, the only way to know for sure is to schedule a consultation with your ENT specialist at Maryland ENT!
How Long Do the Results of RhinAer Last?

From a clinical study, 96% of RhinAer patients reported improved or eliminated symptoms a year after treatment. 88% of patients had improved chronic rhinitis symptoms in a two-year follow-up.
This demonstrates that results from RhinAer are long-lasting and are helping patients get the relief they need from chronic rhinitis. However, results may vary by patient.
Most RhinAer patients will see the full effect of the treatment within four weeks of undergoing RhinAer. You may experience temporary congestion, increased sensitivity, and crusting where you receive treatment for 2 to 6 weeks after treatment.
These are signs that your nasal passage is healing. For the best results, avoid blowing your nose for the first week after your RhinAer treatment, and use any recommended nasal sprays and rinses as directed by your ENT specialist.
Are you ready to find out if you could be a good candidate for RhinAer? Schedule your consultation at Maryland ENT at one of our five convenient locations today!
VivAer
Do you suffer from nasal congestion that hasn’t responded well to medication? Are you looking for a solution that doesn’t involve surgery? VivAer may be an option that will provide you with the relief you need with a non-invasive office-friendly treatment now offered at Maryland ENT.
What is VivAer?

VivAer is a non-invasive procedure that helps reduce nasal airway obstruction (NAO) in patients struggling to breathe. VivAer treatment delivers long-lasting relief from the frustrating symptoms that come with nasal airway obstruction, like congestion, reduced airflow, finding it challenging to exercise, difficulty sleeping, or frequent mouth breathing.
How Does VivAer Work?
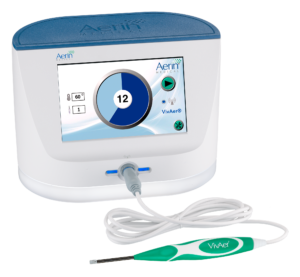
During a VivAer treatment at Maryland ENT, your ENT specialist will begin by applying anesthesia to numb the inside of your nose. After numbing your nose, they insert a small wand into your nostril.
The wand precisely and accurately targets the blockage to treat it efficiently. The tip of the wand uses low-temperature radiofrequency (RF) energy.
Radiofrequency energy helps rebuild your nasal passage in any areas of obstruction to improve airflow in and out of your nose. VivAer is a single-solution, minimally invasive procedure that treats the entire nasal valve.
It increases nasal valve radius to improve airflow and shrinks the inferior turbinate submucosal tissue while reducing soft tissue obstruction on the septum. During VivAer, you will experience minimal discomfort.
There is no lengthy recovery period, allowing you to return to your usual routine almost immediately.
Is VivAer Treatment Long Lasting?
Yes. Clinical studies have shown that after receiving VivAer, patients continued experiencing relief four years after treatment. In a follow-up study, patients experienced improvements across a broad set of quality of life (QOL) measures.
On the NOSE Scale (nasal congestion, nasal blockages, difficulty breathing, trouble sleeping, and inability to get enough air while exercising), patients saw improvements across all 5 QOL measures.
Am I a Good Candidate for VivAer?
Do you struggle with congestion that over-the-counter medications haven’t helped? Have you undergone other surgical procedures to improve your breathing without success?
The only way to know if you’re a good candidate for VivAer is to schedule an appointment at Maryland ENT. However, you can take two simple tests in the meantime to get a better understanding.
Cottle’s Maneuver
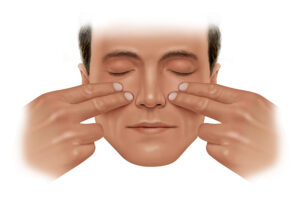
For this test, start by placing two fingertips on your cheeks. Your fingertips should be on each side of your nose. Next, gently press and pull out to further open your nasal passages.
While continuing to hold your fingers in place, breathe through your nose. Did doing the Cottle’s Maneuver help you improve your breathing? If this is the case, you may be a good candidate for VivAer.
NOSE Score
Fill out the NOSE Score to determine if you may benefit from VivAer treatment. If you have a NOSE Score of 55 or higher, this indicates that you have moderate to severe nasal airway obstruction. Patients with this level of obstruction are often excellent candidates for VivAer.
Are you ready to start breathing better? Schedule an appointment at Maryland ENT at one of our five convenient locations to learn more about VivAer, and if it’s a treatment you may benefit from.
Looking for sinus treatment? Learn more by requesting an appointment with the sinus specialists at Maryland ENT in Lutherville and Baltimore, MD today!